The Causes, Types, and Treatments of Achilles Tendon Injuries
Tendons are fibrous tissues that connect muscles with bone. The Achilles tendon is the largest tendon in the body. It connects the calf muscles at the back of the leg with the heel, and facilitates movements such as jumping, running, and walking.
Because the Achilles tendon is engaged so frequently and bears a great deal of pressure and stress throughout the day, it can become injured. Achilles tendon injuries cause the tissue to become irritated, inflamed, and swollen. Pain can come on gradually or be immediate, and will vary from mild to severe depending upon the injury. Where the pain occurs will vary as well, from just above the heel up through the back of the leg. There may also be stiffness in the tendon.
Achilles tendon injuries can often be caused by repetitive stress. They may also occur while running, playing tennis, gymnastics, football, basketball, dancing, soccer, baseball or other sports that require speeding up, slowing down, or pivoting quickly. Wearing high heels, falling from an elevation, stepping in a hole, having flat feet, bone spurs, tight leg muscles or tendons, wearing improper athletic shoes, exercising on uneven surfaces, or starting a new type of exercise can also cause Achilles tendon injuries.
The two most common Achilles tendon injuries are tendonitis and ruptures. Tendonitis causes painful inflammation and can occur in different parts of the tendon. Non-insertional Achilles tendonitis occurs when the fibers in middle of the tendon begin to break down, thicken, and swell. This condition typically affects younger, more active adults. Insertional Achilles tendonitis occurs where the tendon inserts into the heel bone. It is common for bone spurs to form with this type of injury. This condition can affect people of any age and level of activity.
Achilles tendon ruptures are a tear in the tendon. These breaks may be partial or complete. There may be an audible popping noise at the moment of injury and the pain will be sudden and severe.
An Achilles tendon injury can be diagnosed by your podiatrist after they examine you, check your range of motion, and possibly perform a calf squeeze test or review an X-ray or MRI. Depending on the type and severity of your injury, your podiatrist may treat your condition with rest/ice/compression/elevation (RICE), nonsteroidal anti-inflammatory medications, heel lifts, and stretching and strengthening exercises. If you have torn your Achilles tendon, treatment may include physical therapy, ultrasound, shockwave therapy, or possibly even surgery.
Foot Complications From Diabetes
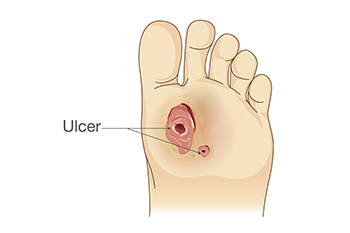
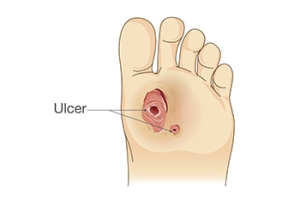
Diabetic foot ulcers and neuropathy are serious complications of diabetes that can lead to infection, hospitalization, or even loss of limbs if left untreated. Neuropathy, or nerve damage, reduces sensation in the feet, making it difficult to feel pain, heat, or injuries. This numbness increases the risk of unnoticed wounds, which can develop into open sores called ulcers that are slow to heal. These ulcers often occur on pressure points like the ball of the foot or heel. Symptoms may include redness, swelling, drainage, and, in severe cases, a foul odor. Some people may not feel any pain due to the loss of sensation, which can delay treatment. A podiatrist will examine your feet, assess circulation, and possibly use diagnostic tools like X-rays or vascular studies. Treatment may involve wound care, custom footwear, antibiotics, and offloading pressure from the affected area. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can help you to manage this serious condition.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Monique Mitchell, DPM from Family Foot Centre. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Garden Hills, Nassau, Bahamas . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Conditions
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
Symptoms and Risk Factors for Sesamoiditis
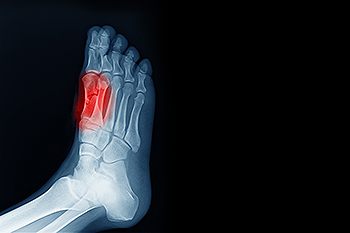
Sesamoiditis involves inflammation of the tendons that surround two small bones located beneath the big toe joint. These sesamoid bones help bear weight and assist with movement, but repetitive stress from running, dancing, or wearing tight shoes can irritate them. People with sesamoiditis often experience a dull, aching pain under the ball of the foot that worsens with activity. The big toe may become stiff or painful to move, and, in some cases, swelling or bruising can develop. A podiatrist can evaluate pain under the toe by checking joint movement and using X-rays or MRI scans to confirm inflammation or rule out fractures. If symptoms do not improve, a podiatrist may suggest orthotic shoe inserts, or, in rare cases, surgery to remove one of the bones. Preventing long-term joint damage requires early diagnosis and care. If you have pain under the big toe, it is suggested that you schedule an appointment with a podiatrist for an exam and appropriate treatment.
Sesamoiditis is an unpleasant foot condition characterized by pain in the balls of the feet. If you think you’re struggling with sesamoiditis, contact Monique Mitchell, DPM of Family Foot Centre. Our doctor will treat your condition thoroughly and effectively.
Sesamoiditis
Sesamoiditis is a condition of the foot that affects the ball of the foot. It is more common in younger people than it is in older people. It can also occur with people who have begun a new exercise program, since their bodies are adjusting to the new physical regimen. Pain may also be caused by the inflammation of tendons surrounding the bones. It is important to seek treatment in its early stages because if you ignore the pain, this condition can lead to more serious problems such as severe irritation and bone fractures.
Causes of Sesamoiditis
- Sudden increase in activity
- Increase in physically strenuous movement without a proper warm up or build up
- Foot structure: those who have smaller, bonier feet or those with a high arch may be more susceptible
Treatment for sesamoiditis is non-invasive and simple. Doctors may recommend a strict rest period where the patient forgoes most physical activity. This will help give the patient time to heal their feet through limited activity. For serious cases, it is best to speak with your doctor to determine a treatment option that will help your specific needs.
If you have any questions please feel free to contact our office located in Garden Hills, Nassau, Bahamas . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Sesamoiditis
Sesamoiditis is a condition that affects the joint that is just behind the big toe in the area known as the ball of the foot. It is most common in younger people and people who have just begun an exercise program. Since the sesamoid bones are like a pulley controlling the big toe, they can rub against each other and cause a gradual onset of pain. Pain may also be caused by the inflammation of tendons surrounding the bones. If ignored, sesamoiditis can lead to other, more serious problems such as severe irritation and fractures of the bones.
The cause of sesamoiditis is sudden increase in activity. The ball of your foot acts as a springboard to help you lift off when you are jogging or running. Sudden increase in the use of these bones or the tendon that controls them can cause irritation. The tendon then begins to develop inflammation and the joint begins to swell. People with smaller, bonier feet or those with a high arch are typically more susceptible to this condition.
Sesamoiditis is fairly simple to diagnose since the symptoms have a gradual onset rather than a sudden impact. The symptoms begin with slight irritation around the joint shortly after the increase in activity. The discomfort eventually turns to pain with light swelling and possibly redness. Although redness or bruising are rare, this may be a symptom. After each session of exercising, the aggravated joint becomes more irritated and increases into a very intense throbbing.
Treatment for sesamoiditis can vary depending on the severity of the situation. However, treatment is almost always approached in a noninvasive way. For a case that is just beginning the doctor may recommend a very strict rest period that will limit the activity allowed on the joint. If you must be active, a recommendation for as modified shoe or insole, along with bandaging and immobilizing the big toe will be made to ensure that pressure is not placed on the joint. For severe cases, it is typically recommended that the joint and the big toe be completely immobilized to allow adequate time to heal. Ice and an over the counter anti-inflammatory may can help with the pain and discomfort while you are at rest.
When you return to your regular exercise activities, it is recommended that you use an insole that will allow even distribution of impact to your entire foot, rather than just the balls of your foot. This will prevent further aggravation of the injury.
Understanding Gait Disorders in Older Adults

As people age, changes in strength, balance, vision, and joint health can lead to gait disorders that increase the risk of falls and limit independence. A gait disorder may involve shortened steps, shuffling, unsteadiness, or asymmetrical walking patterns. These issues can stem from arthritis, neurological conditions, foot deformities, or muscle weakness. Pain in the feet or ankles often contributes to altered walking habits that place strain on other parts of the body. Early identification is important, as many gait disorders can be improved with targeted exercises, proper footwear, assistive devices, or custom orthotics. A podiatrist can evaluate foot mechanics and recommend ways to improve stability and comfort. Regular foot exams are especially important for older adults to detect changes before they lead to serious complications. If walking has become more difficult or unsteady, it is suggested that you schedule an appointment with a podiatrist for a full assessment and treatment options.
If you need your feet checked, contact Monique Mitchell, DPM of Family Foot Centre. Our doctor will attend to all of your foot and ankle needs and provide you with quality treatment.
Geriatrics and Podiatry
When people age, some common issues that may occur are bone density loss, dry skin, poor circulation, and rough brittle nails. These issues may also affect your foot health if the necessary steps are not taken to alleviate the problems.
It is important to take care of your feet because feet that are injured or diseased can affect your overall health. Having painful feet hinders your ability to do daily activities or may decrease your willingness to do the things that you need to do.
Visiting Your Geriatrician
As we age, health problems become more likely, so it is essential to visit your doctor for check-ups to ensure that you are doing the best you can to take care of your health. It is recommended to check your feet frequently for any possible cuts, bruises, swelling, corns or any other irregularities.
Taking Care of Elderly Feet
Cracked or dry feet can be treated by applying moisturizer often. It is also important not to wear old socks because the older the sock is, the higher the possibility there will be that there is bacteria there. Wear fresh socks and make sure they fit properly.
Proper foot health means that you can have a more active lifestyle and you will not be bogged down by pain. Foot health also leads to good circulation, which is paramount for overall health.
If you have any questions, please feel free to contact our office located in Garden Hills, Nassau, Bahamas . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Geriatrics and Podiatry
Bone density loss, dry skin, poor circulation, and rough and brittle nails are some of the common problems that can occur as people age. The effect that these problems has on foot health should be of particular concern in comprehensive geriatric care.
Feet that are diseased or injured have a negative effect on overall health and safety. Painful feet limit a person’s willingness and ability to stay active. Poor foot health can also cause gait change, which can lead to falls and accidents. Even though recovery time from health problems naturally slows as we age, many foot problems can be avoided altogether with regular prophylactic care.
Feet should be thoroughly washed in warm water daily. Care must be taken to dry the feet well, making sure to dry between and under the toes. Any left-over moisture can cause problems like foot fungus. After cleaning feet carefully check for problems such as cracked skin, bruises, swelling, cuts, corns, or other irregularities.
Examine toenails for ingrown, jagged, or split nails. Long toenails should be cut straight across. Never cut toenails at an angle or down the side as this may lead to ingrown nails.
Cracked and dry feet should be treated once or twice a day with a non-greasy moisturizer. Rub the moisturizer into the skin and allow it to dry before putting on socks and shoes. Sweaty feet can be dusted with a small amount of talcum powder. Avoid putting talcum directly into shoes as this may make feet slip within the shoe and cause a serious fall.
Wear clean dry socks each day. Not only do clean socks feel better on the feet, but socks worn for longer periods may harbor disease and odor-causing bacteria. Socks should not be tight around the top as they can leave marks on the leg. Socks that are too small can bring about bruising caused by pressure against the toes.
Wear comfortable and well-fitting shoes. If possible, consult a professional footwear specialist when purchasing shoes. Do not walk around barefoot as this exposes the feet to possible injury and bacteria.
Good foot health allows a more active lifestyle, which improves blood flow. Good circulation aids in recovery from injury or illness. It is also important for maintaining overall health.
Serious health problems can manifest themselves as symptoms in the feet. The elderly should seek professional help from a podiatrist if experiencing foot problems like tingling, numbness, pain, infection, or a sore that does not heal. Taking care of these problems right away can prevent the development of severe cases.
Foot Stretches for Mobility and Strength

Foot stretches play a key role in maintaining healthy, flexible, and strong feet. Regular stretching improves circulation, reduces tension, and enhances mobility. Toe raise, point, and curl exercises strengthen the small muscles in the feet, promoting stability and balance. Toe splays help improve control and coordination, which can reduce the risk of falls and promote better foot alignment. Toe extension stretches are particularly beneficial for those with plantar fasciitis, as they help ease tension in the arch and heel. These simple movements are especially helpful for individuals who spend long hours standing or walking. By incorporating foot stretches into a daily routine, people can maintain better foot health, improve overall posture, and prevent cramping, stiffness, or discomfort. If you have foot pain, it is suggested that you consult a podiatrist who can treat various foot conditions, and guide you on additional effective foot stretches.
Why Stretching Is Important for Your Feet
Stretching the feet is a great way to prevent injuries. If you have any concerns with your feet consult with Monique Mitchell, DPM from Family Foot Centre. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Stretching the Feet
Stretching the muscles in the foot is an important part in any physical activity. Feet that are tight can lead to less flexibility and make you more prone to injury. One of the most common forms of foot pain, plantar fasciitis, can be stretched out to help ease the pain. Stretching can not only ease pain from plantar fasciitis but also prevent it as well. However, it is important to see a podiatrist first to determine if stretching is right for you. Podiatrists can also recommend other ways to stretch your feet. Once you know whether stretching is right for you, here are some excellent stretches you can do.
- Using a foam roller or any cylindrical object (a water bottle or soda can will do), roll the object under your foot back and forth. You should also exert pressure on the object. Be sure to do this to both feet for a minute. Do this exercise three times each.
- Similar to the previous exercise, take a ball, such as a tennis ball, and roll it under your foot while seated and exert pressure on it.
- Grab a resistance band or towel and take a seat. If you are using a towel, fold it length wise. Next put either one between the ball of your foot and heel and pull with both hands on each side towards you. Hold this for 15 seconds and then switch feet. Do this three times for each foot.
- Finally hold your big toe while crossing one leg over the other. Pull the toe towards you and hold for 15 seconds. Once again do this three times per foot.
It is best to go easy when first stretching your foot and work your way up. If your foot starts hurting, stop exercising to ice and rest the foot. It is advised that you then see a podiatrist for help.
If you have any questions, please feel free to contact our office located in Garden Hills, Nassau, Bahamas . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Stretching Your Feet
Debilitating foot pain is a problem for many people. But just as stretching the torso can help alleviate back pain, stretching the feet can also help mend existing foot problems and prevent future ones.
The feet, as the body’s foundation, carry the body’s entire weight and can get easily strained from overexertion. Persistent sharp pain and cramping in the feet are often common concerns. Foot pain and foot problems can be due to any number of causes, and in many cases pain may be eased without medication or doctor visits. It is always a good idea, however, to first rule out any serious medical issues with a physician.
Stretching can help relax the feet and alleviate pain, but is especially important before heavy aerobic exercise. Stretching before such activities can help you avoid experiencing painful cramps or strained foot muscles. Stretches should be performed slowly and deliberately without forceful pulling. The stretch should be held for several seconds before relaxing.
A great way to stretch out and loosen up the foot muscles while sitting is to cross one leg over the other and pull the toes carefully back without overextending. Start by resting the left ankle on the right knee. With the left hand, gently flex the left foot by pulling back on the toes. Do not pull too hard; just hard enough to feel the stretch in the arch of the foot. Then point the toes of the left foot as far as you can. Rotate the motion of pointing with pulling back on the toes. This should relax and stretch the muscles on the bottom and the top of the foot. Doing this stretch ten to twenty times should bring relief. Repeat the whole process for the other foot by resting the right ankle on the left knee.
A stretch that focuses on the often injured Achilles tendon involves standing and facing a wall with your arms out and hands flat against the wall. Step back with one foot, keeping it flat against the floor. Move the other leg forward and lean toward the wall. You should feel a stretch through the back of your leg and your Achilles tendon, but do not push yourself too much. Stop when you feel a stretching sensation, and hold for 30 seconds. Ten repetitions may be done for each foot.
Stretching the feet is important for athletes or those performing aerobic exercise, but it can also help anyone with foot pain caused by poor footwear, plantar fasciitis, or long hours standing and walking. Individuals who tend to their feet by regularly stretching every day should be able to minimize foot pain and prevent new problems from arising.